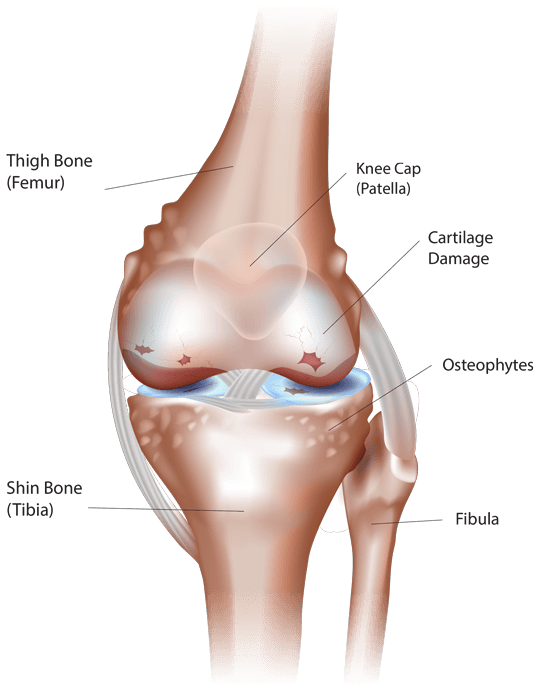
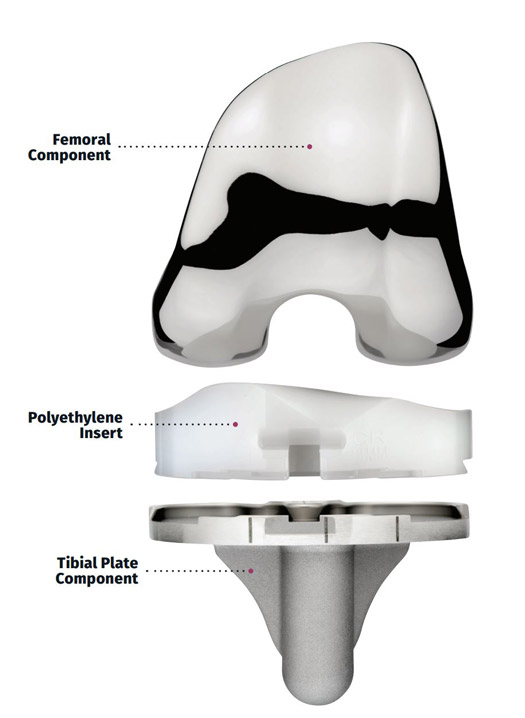
Osteoarthritis affects nearly 350 million people worldwide.1 Those with osteoarthritis of the knee may experience pain, which may keep them from performing and enjoying simple daily activities. In order to treat this condition, your doctor may recommend you have knee surgery with a knee implant manufactured by MicroPort Orthopedics Technology, Inc. Facing surgery can be daunting. However, MicroPort Orthopedics has decades of experience producing revolutionary products which may improve the lives of patients such as yourself, struggling with pain and unable to live the active lifestyle you once did.
Patient resources
PRECAUTIONS & DISCLAIMERS
Every patient is different, and individual results will vary. There are risks and recovery times associated with surgery. Consult your doctor to determine if joint replacement surgery is right for you.
Individual results and activity levels after surgery vary and depend on many factors including age, weight and prior activity level. There are risks and recovery times associated with surgery and there are certain individuals who should not undergo surgery. Please click here to read about risks associated with surgery. Only a physician can tell you if this product and associated procedure are right for you and your unique circumstances. Please consult with a physician for complete information regarding benefits, risks and possible outcomes.